There are treatments and resources designed to provide you with the help and support you may need to get the sleep you deserve.
A bad night’s sleep can happen to anyone. But when you suffer from post-traumatic stress disorder (PTSD), a bad night’s sleep is more common than not. According to research from the Department of Veterans Affairs (VA), 90% of those with PTSD have insomnia and other sleep disorders which are often listed as part of a PTSD diagnosis.
Maybe you’re losing sleep because you’re waking up every night from recurring nightmares. Or maybe you’re unable to relax enough to fall asleep in the first place. Regardless of what’s keeping you awake, poor sleep can take a toll on your physical and mental health and prevent you from successfully treating your PTSD.
Learn more about the connection between sleep issues and PTSD, why good sleep is so important, and what strategies and resources you can use to improve yours.
What Is the Connection Between Sleep Issues and PTSD?
Sleep issues are especially common among Veterans who have been diagnosed with PTSD and can involve a wide range of conditions, such as insomnia, nightmares and obstructive sleep apnea. According to VA, because people with PTSD may try to push away trauma memories during the day, it may cause worries to get worse at night and disrupt sleep. Here are some common examples of how PTSD can interfere with sleep:
- Hyperarousal or the inability to relax – This often presents itself as insomnia and can make it hard to fall or stay asleep. It also makes it more likely that you’ll startle awake because you’re always on alert or listening for danger.
- Intrusion – This may show up as nightmares or night terrors. These intrusive thoughts are often repetitive and related to your past trauma.
- Obstructive sleep apnea – It’s not totally clear why, but this breathing problem is more common in Veterans with PTSD and disrupts your normal sleep.
- Avoidance – People with PTSD may avoid going to sleep. It may feel pointless if it takes hours to fall asleep or it may feel unsafe if you’re waking up with nightmares regularly.
- Increased arm and leg movement – After experiencing a trauma, people may feel more restless and move more during sleep. This may be from enacting a dream or being unable to completely relax.
- Not liking silence – Some people with PTSD may be uncomfortable in complete silence. This may cause you to leave a TV on all night which can disrupt your deepest level of sleep.
Why Is Good Sleep So Important?
Quality sleep is important for a wide variety of reasons – especially when you’re dealing with PTSD or another mental health condition. Here are some of the ways poor sleep may impact your health and wellness:
- Increased risk for additional mental health issues – According to VA, sleep and mental health go hand in hand. If sleep disorders go untreated, they can interfere with recovery or possibly trigger other mental health conditions.
- Effectiveness of your PTSD treatment – Treating both PTSD and sleep conditions together has been more successful than trying to treat the conditions separately. Sleep problems can slow down the recovery process after traumatic events because they interfere with the ability to process memories and emotions.
- Slow reaction time
- Trouble with learning and memory
- Feeling irritable and mood problems
- Trouble with thinking and concentration
- Thinking about suicide or acting in ways that may self-harm
- Increased risk for heart disease, depression, high blood pressure, diabetes, stroke, obesity and more (when sleep issues occur over a long period of time)
What Strategies Can I Implement to Help Me Sleep?
For people who struggle with severe nightmares or for those who have dealt with insomnia for a really long time, it may feel like some of these strategies seem too small in scale to compare to what you’re dealing with. For example, you may wonder – how can a simple breathing technique help me cope with a debilitating nightmare? While not all of these strategies will work for you, one or more of them might. The following list is full of tips from VA researchers as well as tips from other sleep experts who understand the importance of treating sleep issues as a core piece of managing your PTSD.
- Create a bedtime routine. A consistent schedule – as best you can – where you go to bed and wake up at the same time every day can help your body get into a good sleep rhythm.
- Create a safe space for sleeping. To sleep well, your body and mind need to feel safe. Think about what that means for you. If you don’t like the dark, make sure you have a night light in place. If you aren’t comfortable in rooms without windows, try moving to a room that has one. Even if it’s not a typical sleep habit, if it makes you feel safe, it’s worth trying.
- Create a productive sleep environment. Once you’ve established how to feel safe, create an environment that helps you sleep. Experts suggest your room should be kept cool and quiet. Blue light from your phone, a TV or a tablet can make it harder for your body and mind to prepare for sleep. If you’re used to the noise of a TV, try something different like a podcast, white noise or a soothing song.
- Get out of bed if you haven’t fallen asleep within 20 minutes. If you spend too long in bed without sleeping, your mind may begin to race, and it could be hours before you fall asleep. Try getting out of bed, going to another room and doing something relaxing – only returning to bed when you feel sleepy again.
- Avoid caffeine, nicotine or excessive amounts of alcohol before bed. Caffeine, even consumed in the late afternoon, can keep you alert well after bedtime. Nicotine produces adrenaline – even if you use it as a way to calm yourself down. With alcohol, your REM sleep is disrupted as your body spends time processing it.
- Exercise regularly. According to the National Library of Medicine, there is accumulating evidence that regular exercise can be an effective part of PTSD treatment. Exercise can help your body tame hyperarousal, improve your mood, reduce anxiety, and improve your sleep quality and duration.
- Avoid stressors before bedtime. Attempting to fall asleep when you’re agitated or stressed isn’t productive, so try to avoid things that you know may cause those feelings. Think about things that may trigger you, like loud sounds from a TV or a news story about current events that upset you. Give yourself a break from these things and instead use the time before bed to focus on things that help you calm down and unwind.
- Try meditation, deep breathing or another relaxation technique. Learning how to slow your heart rate and calm racing thoughts can be extremely helpful before you fall asleep or after you wake up from a nightmare. VA also recommends the progressive muscle relaxation technique, which involves tensing and relaxing 14 different muscle groups.

- Use a calming sound to help you stay asleep. VA’s research shows that sound therapy can help with sleep issues, anxiety and overall mental well-being. Try using a white noise machine or an app to provide you with a constant, calming sound.
- Deal with daytime stress during the day. Everyone, even people without PTSD, can have sleepless nights when weighing difficult decisions, dealing with financial stress or handling a difficult relationship. What stressful things can you work on during the day that can cause you less worry at night?
- Talk to your health care provider about any medications you’re on. For example, certain anti-depressants that are often used to treat daytime symptoms of PTSD can disrupt sleep and cause insomnia. Make sure you understand the side effects of all of your medications.
- Try not to stress about your inability to sleep. Saying things like “I’m never going to fall asleep” or “These nightmares won’t let me sleep” isn’t helpful and can build more anxiety around trying to sleep. Remember, more than 90% of Veterans dealing with PTSD report having sleep issues. It’s normal to experience these challenges and there are steps you can take to get better.
- Avoid short-term coping strategies that can make things worse. Heavy drinking, drug use and even many sleep medications may feel like they provide the best and most immediate relief to your sleep issues, but these strategies can actually worsen your sleep and aggravate or worsen your PTSD symptoms.
What Treatments or Resources Are Available to Help?
Treating your sleep issues doesn’t have to be something you do on your own in your bedroom at night. Talk with your health care provider and learn more about treatments and resources designed to provide you with the help and support you may need to get the sleep you deserve.
- Cognitive behavioral therapy for insomnia (CBT-I) – According to VA, CBT-I improves sleep in 7 out of 10 people who complete treatment, reducing nightmares and the distress related to them as well as problems with insomnia. VA’s research shows CBT-I to be more effective than medication with fewer side effects. CBT-I can be done online, individually or within a group – allowing Veterans to find the best fit for their needs.
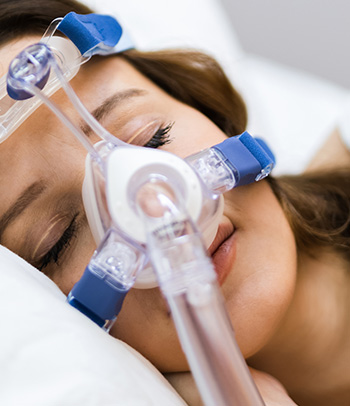
- Positive airway pressure device – This is considered the most effective treatment for obstructive sleep apnea. Since obstructive sleep apnea is often underdiagnosed, health care providers recommend any Veterans with PTSD take a home sleep test.
- Medications – According to VA, sleep medications, including herbal supplements, over-the-counter sleep aids and prescription medications, may provide quick, temporary relief but often only in the short term. Many medications become less helpful over time or begin to cause serious side effects.
- Smartphone apps – VA offers Veterans several digital tools to help them improve their sleep habits. The SleepEZ course and app can help you set a sleep schedule, track your sleep behaviors and eliminate unhelpful thoughts. VA’s Insomnia Coach app provides you with a weekly training plan, a sleep coach for personal feedback, an interactive sleep diary and more. Both of these apps are based on CBT-I and can be used alongside therapy.
- MakeTheConnection – Take a look at other Veterans’ stories about their sleep troubles and the treatments that helped them get back on track.
By addressing your sleep issues as part of your PTSD treatment, you’re likely to see better results. If you have PTSD and your quality of sleep is suffering, speak with your health care team and develop a treatment plan that gets you the rest you need to live well and thrive.







